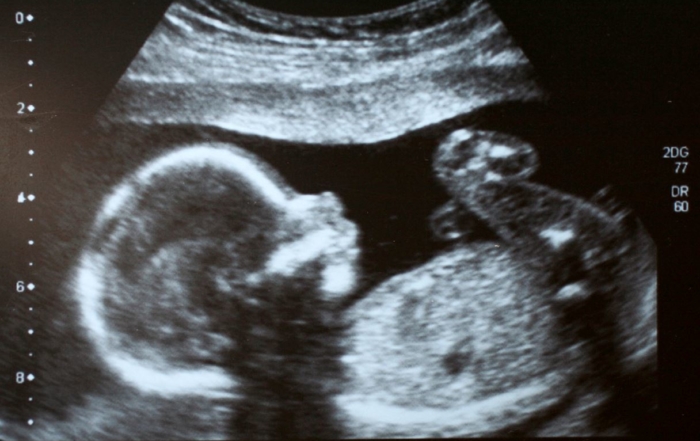
A recent study from researchers at the University of North Carolina reports that the children of depressed mothers treated with selective serotonin reuptake inhibitors (SSRIs) during pregnancy were more likely to develop Chiari type 1 malformations than were the children of mothers with no history of depression.
What is a Chiari Malformation?
A Chiari malformation (CM) is a condition in which brain tissue in the cerebellum extends into the spinal canal. What exactly causes Chiari malformations is not known; however, it is believed that problems emerge during fetal development when the posterior fossa, the part of the skull which holds the cerebellum, is underdeveloped or too small. The cerebellum and brain stem may be pushed downward through the foramen magnum and into the upper spinal canal.
In the past, it was thought that the condition was rare, occurring in about one in every 1,000 births. However, the increased use of diagnostic imaging has shown that CMs are actually more common. It is actually quite difficult to get a precise estimation of the prevalence of this malformation because most people with CMs have no symptoms, and Chiari malformations are often discovered during the course of diagnosis or treatment for another disorder. Often CMs present only with symptoms in adolescence or adulthood. Type 1 Chiari malformations (the type observed in this study) are the most common type of Chiari malformation and are found in about 3% of the population.
CMs occur more often in women than in men and may be more prevalent in certain groups, including people of Celtic descent. It does appear that genetic factors play a role, and therefore some families which have several members with Chiari malformations.
SSRIs and Chiari Malformations
In this study, the researchers identified all children participating in 3 ongoing neuroimaging studies at the University of North Carolina with MRI imaging obtained between 1 and 2 years of age. (The first study was designed to assess the development of the brain in SSRI-exposed children. The other two studies were observing development in healthy singletons and twins.)
The researchers identified 33 children with prenatal exposure to SSRIs. Sertraline was the most commonly used SSRI (n=25) followed by fluoxetine (n=4), citalopram (n=3), and paroxetine (n=2). They also identified a matched group of 66 children with no history of maternal depression and no SSRI exposure. Chiari malformations were found in 18% of the children of mothers who took SSRIs during pregnancy versus 2% of the children of healthy mothers with no history of depression and no SSRI exposure (P = .003; odds ratio [OR], 10.32). The risk for CM was the highest for the children born to mothers who also had a family history of depression (P= .002; OR, 38.08), suggesting that genetic factors, as well as environmental exposures, may be at play.
To test the possibility that a history of maternal depression increases risk for CM in the absence of prenatal SSRI exposure, they identified 30 children (18 male and 12 female) whose mothers had a history of depression but did not receive antidepressants during pregnancy. The children of mothers who had received a diagnosis of depression but who did take antidepressants during pregnancy, did not differ from matched comparison children in occurrence of CMs (7% vs. 5%, p=0.75, OR=1.44).
Understanding the Findings
Based on these findings, the authors concluded that SSRI exposure was associated with an approximately ten-fold increase in risk for Chiari malformations. This study is a bit different from previous studies in that it has demonstrated a greater magnitude of risk. (If we look at the studies that documented an association between exposure to paroxetine and cardiovascular malformations, the risk was much smaller, around 1.5-fold.)
The study does have some important limitations. Probably one of the most significant is the sample size; with such small samples, there is a greater risk of random statistical variation and skewed results. In addition, they were not able to control for the severity of maternal depression. Nor were they able to control for other confounding variables, including risky maternal behaviors during pregnancy (e.g. poor nutrition, smoking, alcohol intake, and substance abuse), maternal obesity, and gestational diabetes. We know that these problems are more common in women treated for depression, and we also know that these problems may affect fetal development.
If there was such a large increase in risk, we might expect to see more of a signal in the medical literature. This is the first report to suggest an association between prenatal SSRI exposure and increased risk of Chiari malformation. To the best of our knowledge, there have been no published case reports of this association. It is possible, that because this condition is not easily identifiable without neuroimaging and may not result in symptoms at all or only later in adolescence or adulthood, that we are not aware of many of these cases.
Given the limitations of this study, the authors of this study urge readers to consider the data as preliminary and caution doctors not to change their prescribing practices based on the results of this study. Most importantly, it is important to note that in the case of observational studies, association does not equal causation. So that we can better advise our patients regarding the risks of these medications, we need larger studies to explore this association and to better understand the role that other confounding variables might play.
Ruta Nonacs, MD PhD
Knickmeyer RC, Meltzer-Brody S, Woolson S, Hamer RM, Smith JK, Lury K et al. Rate of Chiari I malformation in children of mothers with depression with and without prenatal SSRI exposure. Neuropsychopharmacology 2014 May 19. [Epub ahead of print]
Read more about Chiari Malformations (Boston Children’s Hospital)